Repeat coronary revascularization has always been found to be increased by routine follow up coronary angiography (FUCAG) in randomized trials done in the era of balloon angioplasty and percutaneous coronary intervention (PCI) with bare metal stents. But there was never any reduction in major clinical events. Myocardial infarction was reduced with angiographic follow up (AF) than with clinical follow up (CF) in BAAS (Balloon Angioplasty and Anticoagulation Study) and TAXUS –IV trials. Previous studies included low risk patients and hence impact of FUCAG in high-risk patients was unclear.
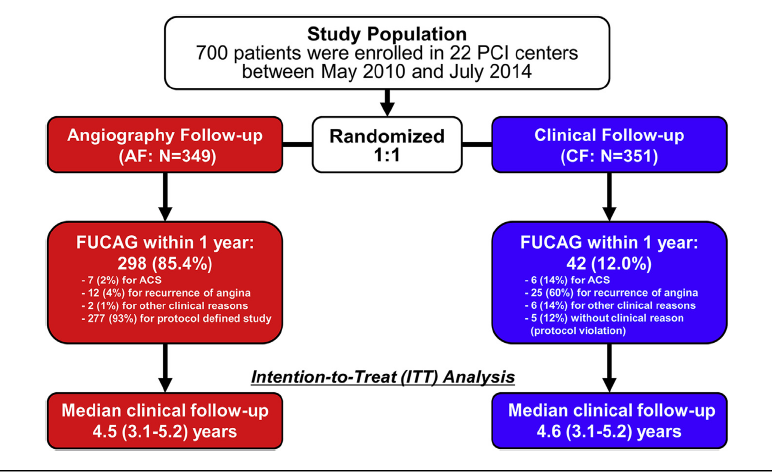
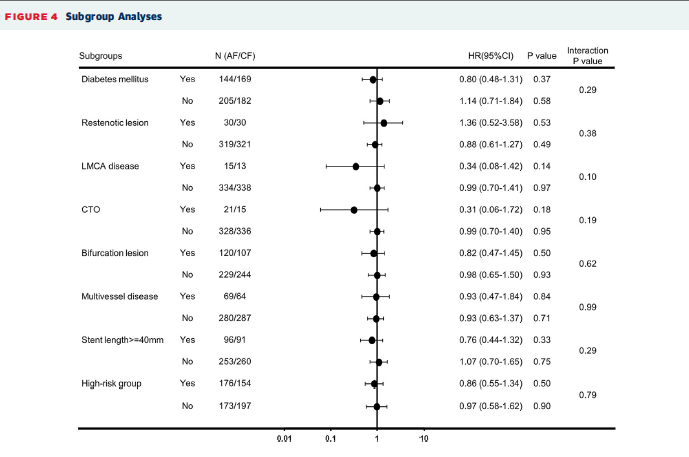
A contemporary study that included 700 high-risk patients has reported that routine FUCAG did not provide any clinical benefits as compared with clinical follow up; and that increased 1 year rate of repeat revascularization with routine angiographic follow up attenuated with long term follow up. There was no preventive effect on incidence of myocardial infarction (J Am Coll Cardiol Intv 2017;10:109-17).
There was also no raised incidence of adverse clinical events with routine angiographic follow up. Therefore angiographic follow up should still be acceptable in the case of a novel stent or device. Routine FUCAG is still performed as usual care in Japan without evidence of any clinical benefit.
“Oculostenotic reflex” is the term coined for coronary revascularization in the absence of objective evidence of ischemia and results in approximately 2-fold higher rate of coronary revascularization as compared with clinical follow up alone. Repeat coronary revascularization was however not significantly higher with routine FUCAG than clinical follow up in a sub-study of the SPIRIT III trial.
Clinical guidelines from the US do not recommend FUCAG even after PCI of left main disease, but current European guidelines regard routine FUCAG in high risk PCI as class IIb.
The current randomized trial was conducted to evaluate the long-term clinical impact of routine FUCAG after PCI in real world clinical practice. The primary endpoint was defined as a composite of death, myocardial infarction, stroke, emergency hospitalization for acute coronary syndrome, or hospitalization for heart failure.
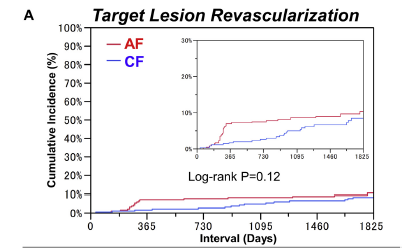
The incidence of the primary endpoint after a median of 4.6 years was 22 % in the angiographic follow up group and 25% in the clinical follow up group (p=0.70). Coronary revascularization was in the first year more frequently performed in the AF group than in the CF group (13% vs. 4%; <0.001). The difference between the 2 groups attenuated over time with similar 5-year incidence (20% vs.18%; p=0.92).
Routine angiography was done at 8 to 12 months following index PCI. Coronary computed tomography was not done in any patient but stress ECG or stress nuclear tests were permitted. Clinically indicated coronary angiography was allowed in acute coronary syndrome, recurrence of angina, and objective evidence of ischemia.